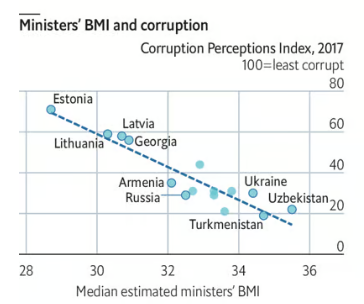
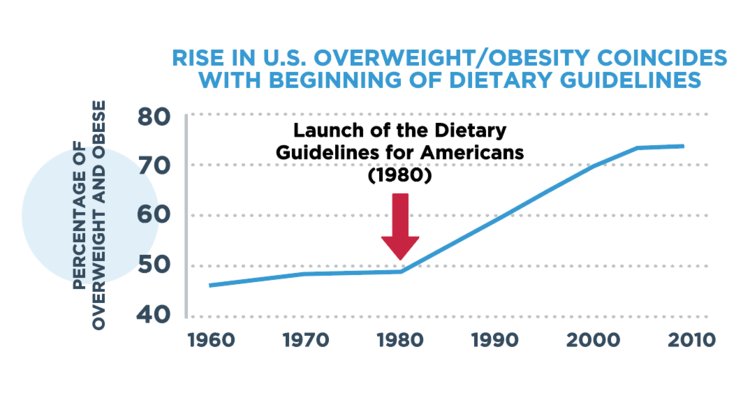
I have been asked to comment on the American Medical Association’s resolution to stop using the BMI as the sole criterion for diagnosing obesity [To find this resolution, click on CCSPH Report(s) #07: Support Removal of BMI as a Standard Measure in Medicine and Recognizing Culturally-Diverse and Varied Presentations of Eating Disorders].
The BMI—Body Mass Index—defined as weight in kilograms divided by height in meters squared—is a quick way to categorize the relationship of weight to height and does a better job of identifying people with excessive body fat than most other simple and inexpensive measures.
Unfortunately, not everyone demonstrates a close correlation of BMI to body fat and those who don’t may well find themselves discriminated against in the health care system.
The BMI is also an imperfect measure of health risk:
The current BMI classification system is also misleading regarding the effects of body fat mass on mortality rates. Numerous comorbidities, lifestyle issues, gender, ethnicities, medically significant familial-determined mortality effectors, duration of time one spends in certain BMI categories, and the expected accumulation of fat with aging are likely to significantly affect interpretation of BMI data, particularly in regard to morbidity and mortality rates…[This report] outlines the harms and benefits to using BMI and points out that BMI is inaccurate in measuring body fat in multiple groups because it does not account for the heterogeneity across race/ethnic groups, sexes, and age-span.
The resolution recommends:
(1) greater emphasis in physician educational programs on the risk differences among ethnic and age within and between demographic groups at varying
levels of adiposity, BMI, body composition, and waist circumference and the importance of monitoring these waist circumference in all individuals with BMIs below 35 kg/m2;
(2) additional research on the efficacy of screening for overweight and obesity, using different indicators, in improving various clinical outcomes across populations, including morbidity, mortality, mental health, and prevention of further weight gain; and
(3) more research on the efficacy of screening and interventions by physicians to promote healthy lifestyle behaviors, including healthy diets and regular physical activity, in all of their patients to improve health and minimize disease risks.
My translation: Keep using the BMI as an indicator, but also pay attention to body composition and waist circumference as better measures of body fat.
The AMA is not minimizing the importance of excess body fat as a disease risk factor. It is saying that only using the BMI to evaluate the risk itself risks stigmatizing patients, especially those of non-majority race, ethnicity, and gender conformation.
This resolution ought to further sensitize physicians to such issues. If it does, it could not come a better time.
Resources
I am putting the Keys’ paper into this discussion to demonstrate that Keys was quite well aware of the strengths and weaknesses of the BMI, which was intended mainly to identify groups and populations at risk of undernutrition.
Guided by the criteria of correlation with height (lowest is best) and to measures of body fatness (highest is best), the ponderal index is the poorest of the relative weight indices studied. The ratio of weight to height squared, here termed the body mass index, is slightly better in these respects than the simple ratio of weight to height. The body mass index seems preferable over other indices of relative weight on these grounds as well as on the simplicity of the calculation and, in contrast to percentage of average weight, the applicability to all populations at all times.