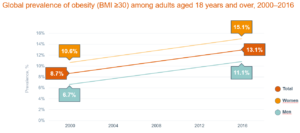
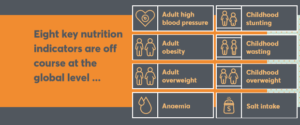
My email inbox was flooded last week with The Obesity Society’s call for more research on the value of taxes on sugar-sweetened beverages.
“Although taxing SSBs might generate revenue that can be used to promote other healthy food items, the net outcome may not necessarily decrease overweight and obesity rates in the United States or worldwide,” said Steven B. Heymsfield, MD, FTOS, President-Elect of The Obesity Society (TOS) and professor and director of the Body Composition-Metabolism Laboratory at the Pennington Biomedical Research Center at Louisiana State University in Baton Rouge.
Why would a professional society that represents people who ostensibly care about obesity science, treatment, and prevention issue a statement aimed at casting doubt on a demonstrably effective public health measure? (Soda companies know the taxes are effective; that’s why they fight them so hard).
The Obesity Society (TOS), alas, often appears far more favorable to the interests of food and beverage companies than those of public health. Could funding of the society and its members have anything to do with this?
Here is the TOS position on corporate funding:
TOS recognizes the value in providing any donor that wishes to support our mission to find solutions to the obesity epidemic the opportunity to provide financial support.
The current TOS policy expressly eliminates all forms of evaluation or judgment of the funding source (other than the stipulation that funding is reasonably assumed not to be derived from activities deemed ‘illegal’).
TOS chooses instead to focus its ethical mission on transparency in disclosing the sources of funding, clear stipulations outlining our commitment to the ethical use of funds, and a commitment to non-influence of the funding sources over the scientific aspects of funded projects and TOS as a whole.
Translation: We will take money from any company, regardless of the effects of its products on public health.
The TOS rationale is that disclosure takes care of the problem and that funding won’t influence the science. Unfortunately for this view, research demonstrates that disclosure does not eliminate the influence of funding, and the influence of funding is considerable—though often unrecognized, as is apparent in this case.
TOS has a disclosure policy, and discloses its officers’ conflicts of interest. These are considerable.
In 2013, Dr. Yoni Freedhoff resigned his TOS membership over the society’s sponsorship policies. In his comment on the current TOS statement, Freedhoff points out that “sugar-sweetened beverage taxes decrease sugar-sweetened beverage consumption and increase healthier beverage consumption while providing the greatest potential health benefits to low income consumers.”
TOS members who care about creating a healthier food environment should consider joining Dr. Freedhoff. lf not, they should insist that TOS leadership take vigorous pro-public health stances on matters affecting their patients’ health.
Additional comments, October 31, 2018
Yesterday I received a message from Liz Szabo, a reporter for Kaiser Health News, who is writing a piece on TOS’s relationships with food companies. She questioned Steve Heymsfield, the group’s current president, who responded at length with a message that included this paragraph:
Marion Nestle, on the other hand, is professor “emeritus” and our understanding is that she no longer reports directly to a dean at New York University. That created a hurdle for us when trying to manage Dr. Nestle’se false and misleading blog related to this matter on her website. Even after learning her comments were misleading from Dr. Popkin, and unlike Popkin who has a high ethical standard, she failed to take down that post.
This surprised me, because nobody from TOS or anywhere else had written me to correct the post, Dr. Popkin’s corrections were to something he—not I—had written, and my ongoing relationship with NYU is readily evident from the information posted under About on this site.
I pointed this out to Dr. Heymsfield, who replied with annotations to my post. Most of these deal with opinion and interpretation rather than fact. The one thing I got “completely false” is my interpretation that TOS lacks standards for deciding which donors are acceptable. Dr. Heymsfield says it does. I am happy to hear that and stand corrected on that point.






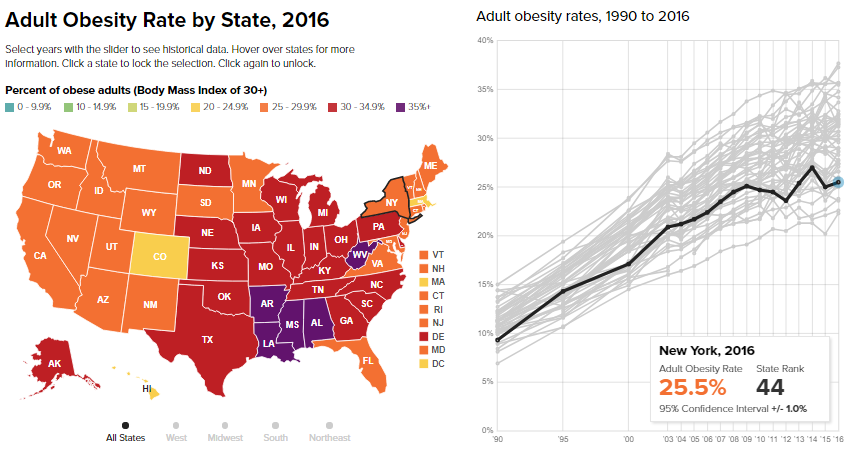
 It also deals with adult obesity:
It also deals with adult obesity: